Meniscal tears: the basics
Menisci are a type of cartilage inside the knee joint.
Their main function is to equally distribute the force placed on the knee, stabilize the knee during movements, and offer more fluid movements.
There are two menisci; one on the outer edge of the knee (called the lateral meniscus), and one on the inner edge of the knee (called the medial meniscus). Tears can occur in either menisci, although they are more likely to occur in the inner (medial) meniscus due to it being more rigidly attached to the medial collateral ligament compared to the outer (lateral) meniscus.
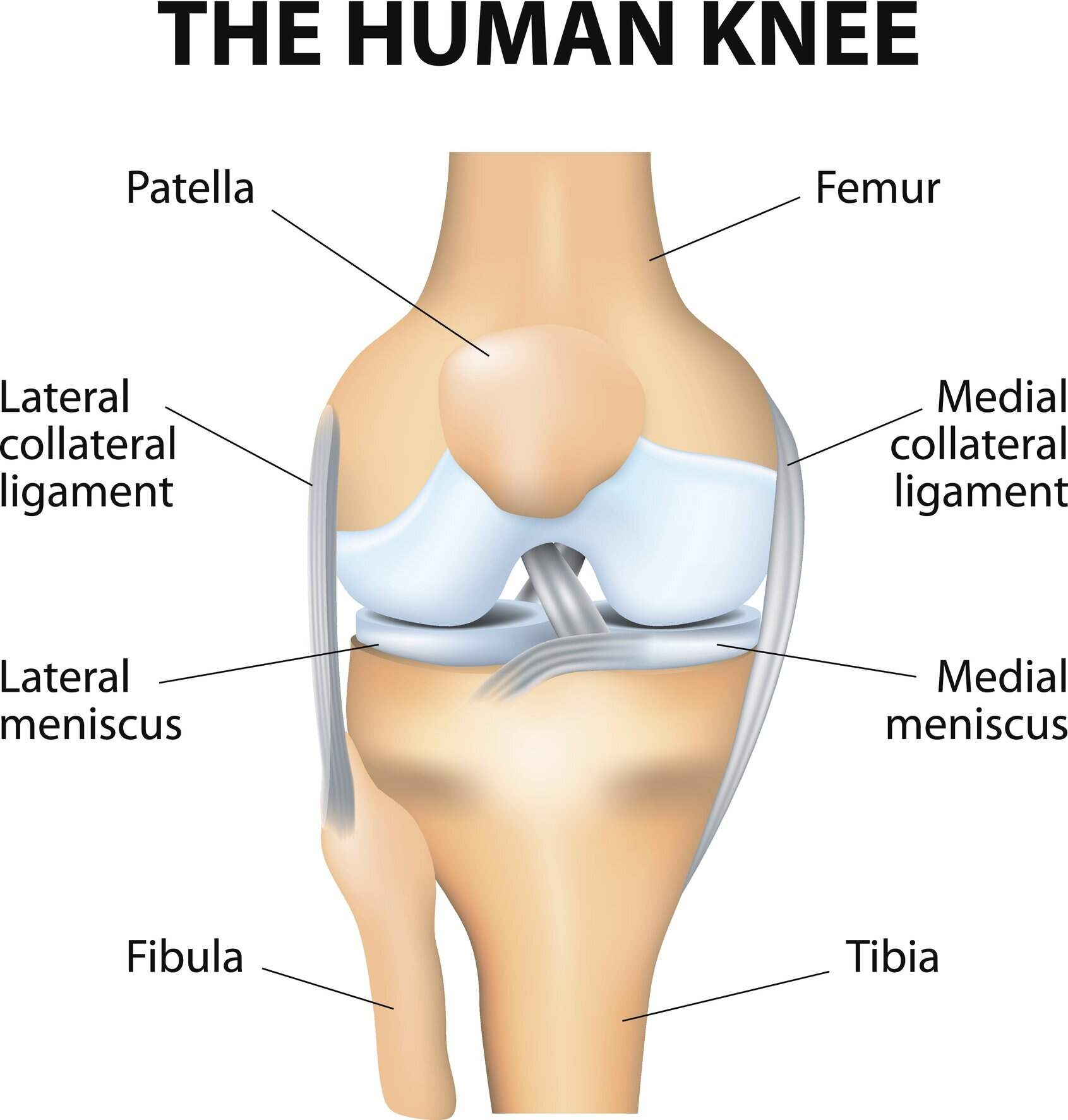
Causes of meniscal tears

Meniscal tears will often result from a “twisting” force on the knee while it is partially bent (flexed). For example, standing up from a crouched position too quickly, falling, twisting or pivoting movements in sports like soccer and basketball, or stopping and changing directions quickly.
In older patients, tears can occur from degeneration of the meniscus as part of the aging process when the collagen fibers begin to disintegrate and provide less support for the knee joint. Frequent kneeling, squatting, or using stairs are also risk factors for developing a degenerative tear.
Types of tears
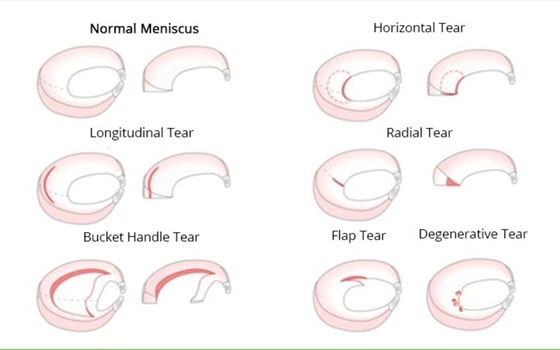
- Radial tears are common. They occur in the area of the meniscus where there is no blood supply and therefore do not heal very well.
- Longitudinal tears heal more easily because they occur in an area of the meniscus with a good blood supply.
- Bucket Handle tears are some of the largest tears and often give the feeling of blocking normal knee movement. These tears usually occur in people aged under 35.
- Flap tears can cause ‘catching’ symptoms in the knee joint that can be described as feeling a “click” or “catch” when bending the knee
- Horizontal (cleavage) tears are the type of tears that most often require surgery as the torn meniscus can limit knee movement
- Degenerative tears are usually found in the back and middle parts of the meniscus.
Symptoms
Meniscal tears cause knee pain immediately following the injury, which can increase in the weeks following the initial trauma. Pain is usually worse when squatting, twisting, or when the knee is bent.
People with a meniscal tear can have difficulty weighting the affected leg, or may experience catching or locking in the knee. Knee locking is when the torn meniscus becomes lodged in the knee joint causing the knee to feel stuck, and making it impossible to fully straighten or bend the knee.
After an injury there may be bruising and swelling around or behind the knee, depending on the location of the tear.
Degenerative tears are one of the first signs of wear in the knee joint and can also be an early indication of osteoarthritis. These tears are most common in people aged 40-60 and usually cause milder symptoms in the beginning, such as knee pain after physical activity, pain when bending the knee fully, and mild swelling. Over time these symptoms can increase, or they will flare up for a few months and then settle down again.
Diagnosis
In addition to the symptoms described above, a physical exam performed by a health professional can help figure out the cause of your knee pain.
Your physician will look for swelling around the knee, pain when the knee joint is compressed or fully bent, as well as increased pain when squatting.
Knee motions may also feel less smooth during the physical assessment if there is a meniscal tear.
Imaging
X-rays are used to look at the amount of space between the bones in the knee joint and are useful in diagnosing degenerative tears.
Magnetic Resonance Imaging (MRI) is the most sensitive test for diagnosing meniscal tears, as well as determining the type and location of the tear. However, MRIs are not usually needed to diagnose meniscal tears, particularly if surgical treatment is not being considered.
Treatment
Non-surgical
If the knee is stable and there is no locking of the knee, initial treatment of meniscal tears will not involve surgery.
Initial treatment typically includes physical therapy, particularly exercises that strengthen muscles around the knee and the quadriceps, pain relief medications, exercising the joint, and icing.
If the knee is swollen and painful, patients should avoid activities like squatting, twisting of the knee, pivoting, kneeling, and repetitive bending of the knee such as climbing stairs, pedaling, jogging, etc…
Surgical
The decision to opt for surgical treatment can be influenced by a number of factors that include:
- the frequency and severity of symptoms
- how much your daily function is affected by symptoms
- if 6-months of non-operative treatment does not improve symptoms
- if you have a complex type of tear
- if you have a horizontal tear as these will rarely heal with non-operative treatment
- the amount of damage to the knee joint surfaces
- age, as there are lower rates of healing due to tissue changes with aging
Options for surgery include:
Meniscectomy – where the torn meniscus is completely removed from the knee joint. This is usually done through arthroscopic surgery where a camera is inserted into the knee joint, minimizing scarring and recovery time. The camera is used by the surgeon to look at the meniscus and then another tool is inserted into the knee to trim the damaged meniscus.
Meniscal repair – where the meniscus is repaired by the surgeon stitching (suturing) the tear together using a camera inside the knee. This surgery can only be used for some types of tears. Repair is usually not possible when the tear is on the inner, thin edge of the meniscus, because there is poor blood supply, making healing of the repair less likely.
Outcomes
Rehabilitation and physical therapy play an important role in meniscal tear recovery regardless of whether or not surgery was required.
Recovery time is usually 6 to 8 weeks with non-operative treatment, and up to 3 months or more with surgery.
In some cases where there is a meniscal tear combined with early or moderate arthritis, it may take a few months to improve symptoms and knee strength.
In addition,
- Meniscus tears often heal well for patients that have non-degenerative tears
- Healing of the meniscal tear is usually improved in patients who are younger than 35 years of age
- Meniscal injuries may predispose to long term development of arthritis. These risks are reduced in meniscal repairs
- Surgical treatment offers a better chance of returning to sport
- If surgery is done, there are generally good outcomes for patients based on a research study that followed up with patients after ten years
Expert Contributor

Laura May Miles, MD(c), LL.M., LL.L. Graduating Medical Student
References
Belzer JP, Cannon WD Jr. Meniscus Tears: Treatment in the Stable and Unstable Knee. J Am Acad Orthop Surg. 1993 Oct;1(1):41-47. doi: 10.5435/00124635-199309000-00006. PMID: 10675855.
Buchbinder R, Harris IA, Sprowson A. Management of degenerative meniscal tears and the role of surgery. Br J Sports Med. 2016 Nov;50(22):1413-1416. doi: 10.1136/bmj.h2212. PMID: 27802970.
Chatain F, Adeleine P, Chambat P, Neyret P; Société Française d’Arthroscopie. A comparative study of medial versus lateral arthroscopic partial meniscectomy on stable knees: 10-year minimum follow-up. Arthroscopy. 2003 Oct;19(8):842-9. doi: 10.1016/s0749-8063(03)00735-7. PMID: 14551546.
Faucett SC, Geisler BP, Chahla J, Krych AJ, Kurzweil PR, Garner AM, Liu S, LaPrade RF, Pietzsch JB. Meniscus Root Repair vs Meniscectomy or Nonoperative Management to Prevent Knee Osteoarthritis After Medial Meniscus Root Tears: Clinical and Economic Effectiveness. Am J Sports Med. 2019 Mar;47(3):762-769. doi: 10.1177/0363546518755754. Epub 2018 Mar 8. PMID: 29517925.
Howell R, Kumar NS, Patel N, Tom J. Degenerative meniscus: Pathogenesis, diagnosis, and treatment options. World J Orthop. 2014 Nov 18;5(5):597-602. doi: 10.5312/wjo.v5.i5.597. PMID: 25405088; PMCID: PMC4133467.
Ma J, Chen H, Liu A, Cui Y, Ma X. Medical exercise therapy alone versus arthroscopic partial meniscectomy followed by medical exercise therapy for degenerative meniscal tear: a systematic review and meta-analysis of randomized controlled trials. J Orthop Surg Res. 2020 Jun 15;15(1):219. doi: 10.1186/s13018-020-01741-3. PMID: 32539864; PMCID: PMC7296921
Ménétrey J, Siegrist O, Fritschy D. Medial meniscectomy in patients over the age of fifty: a six year follow-up study. Swiss Surg. 2002;8(3):113-9. doi: 10.1024/1023-9332.8.3.113. PMID: 12125334.
Patel H, Skalski MR, Patel DB, White EA, Tomasian A, Gross JS, Vangsness CT, Matcuk GR Jr. Illustrative review of knee meniscal tear patterns, repair and replacement options, and imaging evaluation. Clin Imaging. 2021 Jan;69:4-16. doi: 10.1016/j.clinimag.2020.06.045. Epub 2020 Jul 2. PMID: 32650296.
Sihvonen R, Paavola M, Malmivaara A, Itälä A, Joukainen A, Kalske J, Nurmi H, Kumm J, Sillanpää N, Kiekara T, Turkiewicz A, Toivonen P, Englund M, Taimela S, Järvinen TLN; FIDELITY (Finnish Degenerative Meniscus Lesion Study) Investigators. Arthroscopic partial meniscectomy for a degenerative meniscus tear: a 5 year follow-up of the placebo-surgery controlled FIDELITY (Finnish Degenerative Meniscus Lesion Study) trial. Br J Sports Med. 2020 Nov;54(22):1332-1339. doi: 10.1136/bjsports-2020-102813. Epub 2020 Aug 27. PMID: 32855201; PMCID: PMC7606577.
Thorlund JB, Englund M, Christensen R, Nissen N, Pihl K, Jørgensen U, Schjerning J, Lohmander LS. Patient reported outcomes in patients undergoing arthroscopic partial meniscectomy for traumatic or degenerative meniscal tears: comparative prospective cohort study. BMJ. 2017 Feb 2;356:j356. doi: 10.1136/bmj.j356. PMID: 28153861; PMCID: PMC5421436.
Van de Graaf VA, Wolterbeek N, Mutsaerts EL, Scholtes VA, Saris DB, de Gast A, Poolman RW. Arthroscopic Partial Meniscectomy or Conservative Treatment for Nonobstructive Meniscal Tears: A Systematic Review and Meta-analysis of Randomized Controlled Trials. Arthroscopy. 2016 Sep;32(9):1855-1865.e4. doi: 10.1016/j.arthro.2016.05.036. Epub 2016 Jul 27. PMID: 27474105.
Weiss CB, Lundberg M, Hamberg P, DeHaven KE, Gillquist J. Non-operative treatment of meniscal tears. J Bone Joint Surg Am. 1989 Jul;71(6):811-22. PMID: 2745476.







