Achilles tendon rupture: the basics
The Achilles tendon is a tough fibrous band of tissue that attaches the calf muscles to the heel bone. It is the largest tendon in the entire body and the most common tendon in the lower body to rupture.
When the calf muscles flex, the Achilles tendon pulls up on the heel bone and helps us stand on our tip-toes, walk, run, and jump.
We rely on it virtually every time we walk or move our foot. Hence, injuries to the Achilles can be severely debilitating.
The name “Achilles” comes from Greek mythology and its reference to Achilles the Greek warrior in which its stated that his only point of weakness was his heel.

Who is at risk?
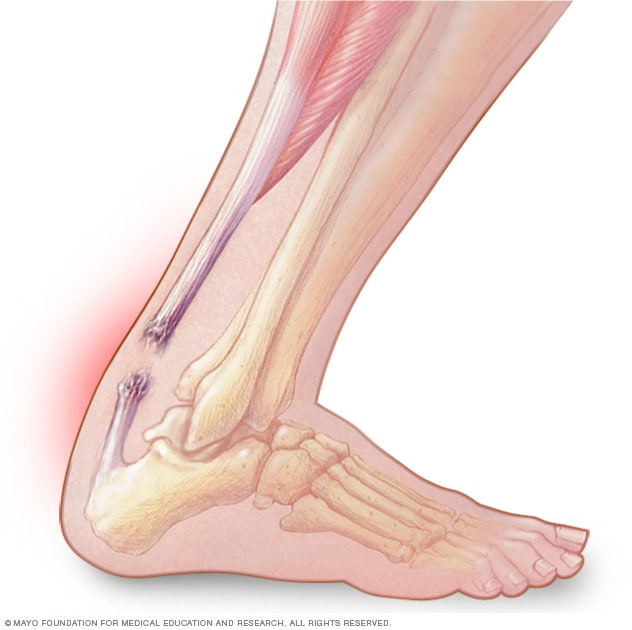
Achilles tendon ruptures are common tendon injuries that happen when a person suddenly bends their ankle toward the shin, when they are trying to plantarflex or point their foot into the ground.
Participation in sport or recreational activity is the most common way to rupture the Achilles tendon – approximately 80% of injuries occur this way! For example, sports where there is running, cutting, jumping or bouncing on one’s feet like a gymnast or a basketball player can increase the risk of having this type of injury.
About 10% of Achilles tendon ruptures occur in people who have pre-existing Achilles tendinopathy (overuse injury).
Rupture can also occur when falling from a height or stepping into a hole.
This injury also commonly occurs in older adults, particularly men in their 40s.
Men are 2 – 8 x more likely to rupture their Achilles tendon than women.
The use of local corticosteroids injections or certain antibiotics called fluoroquinolones have also been shown to increase the risk of having an Achilles tendon tear. Fluoroquinolones have been shown to weaken the proteins and molecules that surround, support, and give structure to the cells around the Achilles tendons which can weaken then tendon. A patient who has multiple corticosteroid injections without taking the appropriate time to rest and recover can cause proteins like collagen to weaken and cause a decrease in blood supply to the Achilles tendon, effectively weakening the tendon as well.
What does an Achilles tendon rupture feel like?

When patients rupture their Achilles tendon they usually describe the feeling of someone hitting or kicking them in the back of the heel, with an associated “pop”. They are then unable to point their foot or walk normally and feel pain in their heel.
Some patients will also describe that their foot feels like it goes through a hole in the floor when jumping or landing.
How is a rupture diagnosed?
The doctor will first ask about the story of how the injury happened. The doctor will then inspect the calf and heel looking for swelling, a gap in the tendon, bruising, and compare it to the other side.
They may ask to see if you can point and flex your feet. Finally, they will do a test called the “Thompson Test” in which you lay on your stomach with your feet off the edge of the bed, and they will squeeze your calf muscles. If they squeeze your calf muscles and your foot points down, this likely means that your Achilles tendon is still attached to your heel bone. If the doctor squeezes your calf muscles and your foot does not move, this makes it more likely that your Achilles tendon is torn.
More imaging may be needed to help rule out other injuries, or to help with a diagnosis. This could include an x-ray, Ultrasound, or MRI.
How is an Achilles tendon rupture treated?
Achilles tendon injuries can be treated with or without surgery.
Studies have shown that in most cases, surgery is not needed for an Achilles tendon rupture if the patient has started an appropriate rehabilitation protocol within a few weeks after injury.
The risk of re-tear in patients that have completed rehabilitation is equal to those of patients who have surgery, without the added risk of surgical complications that can include: infection, blood clot, scarring, and wound complications – although the risk of these complications is very low.
Strength, range of motion, calf circumference, and functional outcomes are also similar between patients regardless of treatment (surgical versus non-surgical).
Despite the treatment choice, one to two years after injury, patients can expect a decrease in function of their Achilles compared to their uninjured side.
In rare case, Achilles tendon ruptures do not heal appropriately. If this is the case, surgery is then recommended.
What to expect from surgery?
If you and your surgeon decide that the surgical route is best for you, you can expect a scar at the back of your ankle and lower leg, just on the inside of where your Achilles tendon outline normally shows through your skin. This is where the surgeon has cut down to your torn Achilles tendon.
The surgeon will find where it is torn, remove any tissue that looks like it won’t heal nicely, and stitch the two ends back together. The surgeon will check to make sure that the tension of the Achilles is back to where it is best for you and then close up your wound with stitches.
After this is complete, you will start at the very beginning of a dedicated rehabilitation protocol.
The first two weeks after injury, you will be in an aircast boot with a 2cm heel lift and will not be putting any weight onto the injured leg. From here you will gradually decrease the heel lifts and gradually return to weightbearing on your injured leg.
Contributing Expert
Jayd Lukenchuk, Orthopaedic Surgery Resident, University of Calgary
References
- Hess GW. Achilles tendon rupture: a review of etiology, population, anatomy, risk factors, and injury prevention. Foot Ankle Spec. 2010 Feb;3(1):29-32 Epub 2009 Dec 15
- Soroceanu A, Sidhwa F, Aarabi S, Kaufman A, Glazebrook M. Surgical versus nonsurgical treatment of acute Achilles tendon rupture: a meta-analysis of randomized trials. J Bone Joint Surg Am. 2012;94(23):2136-2143. doi:10.2106/JBJS.K.00917
- Willits K, Amendola A, Bryant D, Mohtadi NG, Giffin JR, Fowler P, Kean CO, Kirkley A. Operative versus nonoperative treatment of acute Achilles tendon ruptures: a multicenter randomized trial using accelerated functional rehabilitation. JBJS. 2010 Dec 1;92(17):2767-75.