Fixing the Cuff
Banff Sport Medicine Physician, Dr Andy Reed, discusses rotator cuff injuries in his latest Bow Valley Crag & Canyon article.
I see a lot of rotator cuff injuries! In fact, I’d guess about 15-20 percent of all the patients we put through our clinic have a shoulder injury of one kind or another, and if the patient is over age 40, there’s a good chance that they have a rotator cuff problem.
What is the rotator cuff?
The term ‘rotator cuff ’refers to a group of four tendons and their muscular attachments that connect the top of the humerus to the shoulder blade.
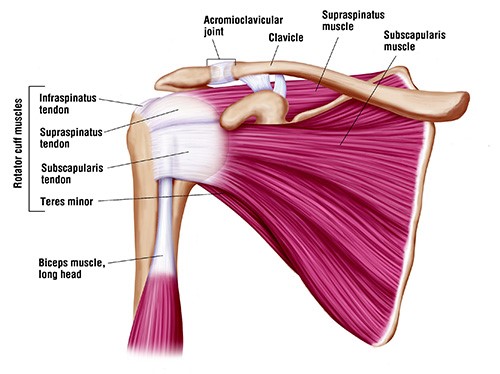
The shoulder socket is a bit like a golf ball sitting on a tee. The cuff helps to hold the ball in the centre of the tee.
The job of the rotator cuff in simplistic terms is two fold; firstly the cuff stabilizes the spherical head of the humerus in the shallow socket of the shoulder blade.
Secondly, the cuff assists in initiating shoulder movements.
If we lift our arm out to the side of the body, we activate our upper cuff. If we reach into our back pocket or rotate our arm backwards to put on a seat belt for example, we are activating our cuff. If our cuff has been injured, these simple motions can become painful and weak.
How does the rotator cuff become injured?
The rotator cuff is a common source of shoulder pain especially in those over the age of 40. The 4 tendons of the cuff are very small – around 6 to 8 mm only, and repetitive shoulder movements can easily irritate or injure these important structures.

The tendons are commonly injured in falls from mountain bikes or in ski wipeouts. They can also become inflamed during overhead sports.
They can begin to deteriorate as we age and sometimes we see tears in tendons that have not been subject to any obvious trauma.
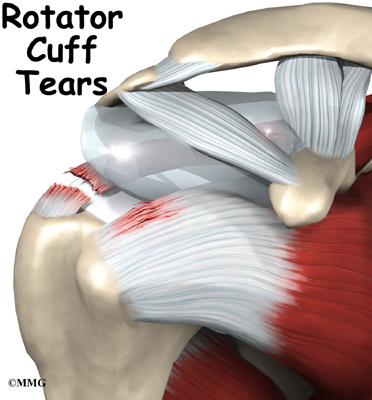
Small bone spurs will commonly form above the cuff on a a part of the shoulder blade called the acromion, and these spurs can rub and irritate the cuff tendons, eventually leading to fraying and ultimately tears.
These are known as degenerative tears. Many of these tears, in fact, cause no symptoms at all, and as many as 50% of the over 50s will have small rotator cuff tears if we go looking for them.
We tend to see cuff injuries in clinic either after falls, when the onset is very sudden, or more insidiously in our older patients. Patients complain of pain when lifting the arm out to the side or during overhead activity. Pain is common at night, and can disturb sleep.
There may also be marked weakness during activity; even seemingly simple activities such as dressing and driving can become limited if pain is severe.
Diagnosis & treatment
We can measure the size and extent of the injury. We can determine if the tendons are torn or just inflamed. We can also scan the shoulder as it moves which provides additional information.
If we determine that the cuff is torn, more imaging may be ordered and this is often in the form of an MR arthrogram, where dye is injected into the shoulder before the MRI. This helps us to see tears in more detail and is helpful at looking for additional problems in the shoulder socket that ultrasound cannot detect.
Almost always we will recommend physical therapy. A skilled therapist can help to get the shoulder moving with less pain. As pain improves, strengthening of the uninjured cuff muscles and tendons can help restore function, and in many cases, complete restoration of full function can be achieved, though these are typically slow injuries to resolve.
In some cases surgery may be needed to repair the damaged tendon, but recovery is lengthy, so we will often begin with non-surgical treatments if there is a good chance that the injury can recover. If pain is severe, we may recommend a steroid injection into the richly innervated bursa that sits above the cuff. This is achieved using ultrasound to ensure that the injection goes into the right place.
We are increasingly using platelet rich plasma injections into small cuff tears to reduce pain and promote healing, and recent studies have shown these to be very safe and more effective than steroid injections. If you are still symptomatic despite these treatments our surgical colleagues will be happy to help!
Overall, rotator cuff tears are very common, and with proper management complete restoration of strength and function can be achieved.
Expert Contributor

Dr Andy Reed, Banff Sport Medicine Physician and ultrarunning M.D.







