Tennis Elbow (Lateral Epicondylitis): the basics
The name “Tennis Elbow” suggests tennis players are highly prone to this particular injury.
While this can be the case due to their wrist bending backwards when they hit the ball, this injury is more common in people who don’t play professional tennis.
Any job or sport which requires frequent backward bending or overuse of the wrist and arm has a potential risk of developing this painful condition.
What is tennis elbow (lateral epicondylitis)?
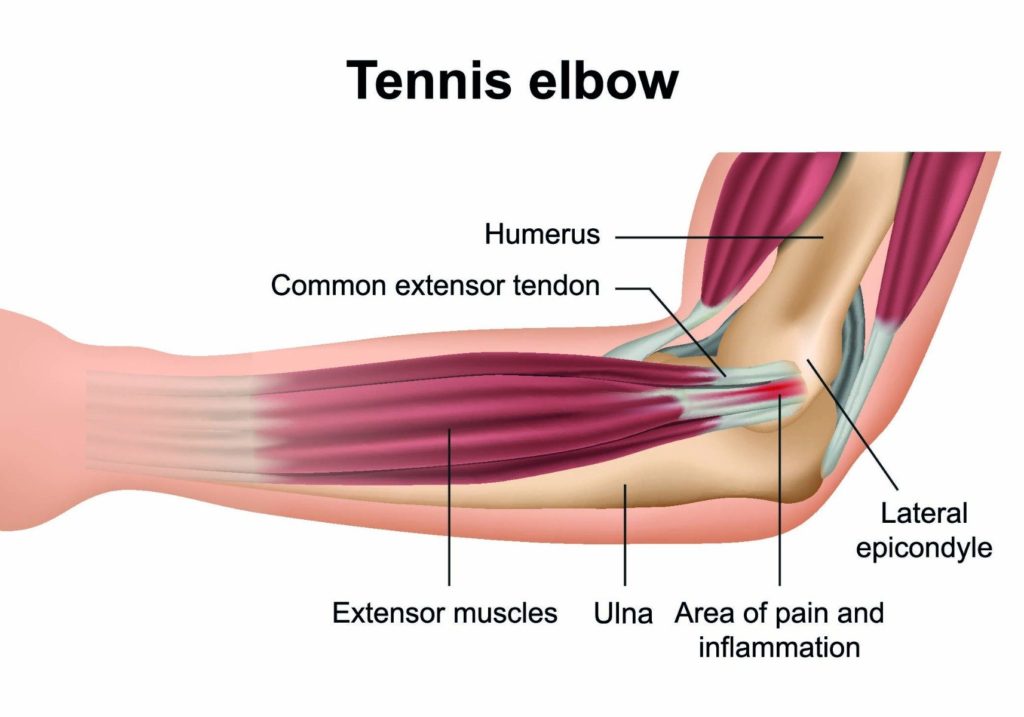
Tennis elbow is an overuse and muscle strain injury that occurs due to repeated contraction of the forearm muscles that are used to straighten and raise your hand and wrist.
Repeated contraction can result in a series of microscopic tears and swelling in the tendons that attach the forearm extensor muscles to the bony part of the outer elbow.
This bony bump on the outer elbow is called the lateral epicondyle. Hence, tennis elbow is also known as “lateral epicondylitis”, which literary means, inflammation of the lateral epicondyle.
Risk Factors for Tennis Elbow
AGE: Most common in people aged 30 to 50, but can occur at any age
OCCUPATION: Plumbers, Painters, Carpenters, Butchers, Cooks
CERTAIN SPORTS in the Bow Valley: Rock climbing, having too wide mountain bike handlebars, and tennis and other racket sports

Symptoms of Tennis Elbow
- Pain and burning on the outer part of elbow leading to worsening movements like shaking hands, squeezing, lifting. Pain usually develops slowly. Sometimes pain occurs at night.
- Weak grip strength – As your grip weakens you may develop difficulty in turning a doorknob, holding a coffee cup etc.
Diagnosis
Your physician will conduct a physical examination and consider several factors that include your occupation and recreational activities.
While physical exam is usually enough to diagnose tennis elbow, your physician may also request additional tests such as:
- X- Ray – To rule out underlying problems with the bone like arthritis that may be causing symptoms.
- Magnetic resonance imagining (MRI) – which can show the damage in the tendon and muscle, as well as its severity.
- Electomyography (EMG) – to rule out compression of the nerve that may be causing elbow pain.
- Ultrasound – Can be used to measure the extent of damage or improvement following treatment.
Treatment
Non-surgical
Most people recover from tennis elbow with non-surgical treatments.
Non-surgical treatments that have shown to be most effective include:
- Rest the muscle group.
- Avoid / modify the activity which causes worsening of pain/symptoms.
- Pain medication such as acetaminophen (Tylenol) or Ibuprofen (Advil) – consult pharmacist for the correct dose and precautions.
- Physiotherapy to strengthen the muscles of the arm.
- Injections in conjunction with physiotherapy, activity modification and bracing may be recommended. Injections include:
- Steroids, such as cortisone, which can effectively relieve pain to allow healing.
- Platelet rich plasma (PRP) can improve healing and may reduce pain.
- Prolotherapy using dextrose as well as freezing to encourage healing and alleviate pain.
- SportVis, which is a new Hyaluronic Acid product with excellent evidence for treatment of acute and chronic tennis elbow.
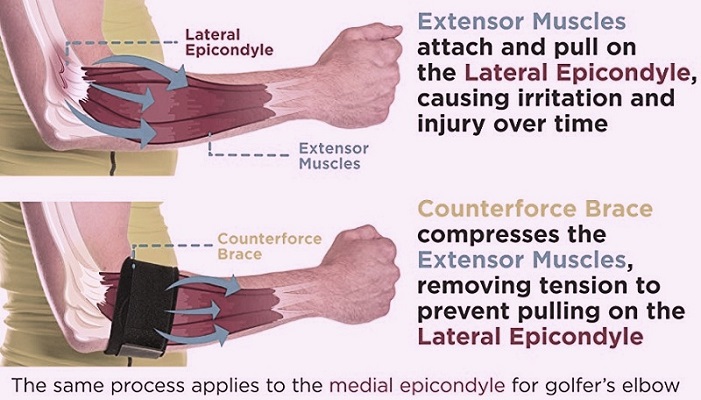
- Bracing, such as a counterforce brace, reduces the pressure on the affected muscles.
Surgical treatment
Surgery is usually recommended for those cases where non-surgical treatments have failed.
Two surgical options exist, both with the same aim of removing the damaged tissue:
- Open Surgery where an incision is made over the elbow.
- Arthroscopic surgery done using a small incision and an arthroscope.
Prevention
Putting less or no strain on the forearm muscles will help avoid the occurrence of tennis elbow or prevent symptoms from getting worse.
Preventative measures include:

- Stopping any action that causes pain or try an alternative way of doing it.
- Strengthening and conditioning of the involved muscles.
- Coaching on proper technique to avoid or minimize the use of the affected muscles and tendon.
- Including a gentle warm up prior to activity.
- Using lightweight tools or racquets, and/or increase grip size, to avoid putting extra load on the tendon.
- Wearing an elbow splint/brace. Consult your physician or physiotherapist for the best type of brace or splint.
Expert Contributor

Dr Ashutosh Vaidya, M.Sc., M.D., PMP, and Banff Sport Medicine Foundation Volunteer!
References
Bisset L, Coombes B, Vicenzino B. Tennis elbow. BMJ Clin Evid. 2011 Jun 27;2011:1117. PMID: 21708051; PMCID: PMC3217754.
Duncan J, Duncan R, Bansal S, Davenport D, Hacker A. Lateral epicondylitis: the condition and current management strategies. Br J Hosp Med (Lond). 2019 Nov 2;80(11):647-651. doi: 10.12968/hmed.2019.80.11.647. PMID: 31707890.
Cutts S, Gangoo S, Modi N, Pasapula C. Tennis elbow: A clinical review article. J Orthop. 2019 Aug 10;17:203-207. doi: 10.1016/j.jor.2019.08.005. PMID: 31889742; PMCID: PMC6926298.
Coombes, Brooke K.; Bisset, Leanne; Vicenzino, Bill (November 2015). “Management of Lateral Elbow Tendinopathy: One Size Does Not Fit All”. Journal of Orthopaedic & Sports Physical Therapy. 45 (11): 938–949. https://doi.org/10.1179%2F106698107791090132 ISSN 0190-6011. PMID 26381484
Lenoir H, Mares O, Carlier Y (2019) Management of lateral epicondylitis. Orthopaedics & Traumatology: Surgery & Research. 105(8): S241-S246 https://doi.org/10.1016/j.otsr.2019.09.004







